New Democrat Coalition Tours Three NIH Labs

Photo: Chia-Chi Charlie Chang
Nine members of the New Democrat Coalition recently visited NIH to tour the Clinical Center (CC). The congressional delegation learned about several cutting-edge research initiatives and gained insight into how new technologies are poised to challenge today’s pressing health issues.
Some were visiting NIH for the first time. All had a vested interest in health care and were eager to learn more about the latest research into cancer, mental health and addiction.
“It’s an opportunity for us to get to know what goes on at NIH, get a tour and speak with leadership,” said Rep. Terri Sewell (D-AL), who chairs the Health Care, Substance Use and Mental Health Task Force.
“Substance use and mental health disorders are a big priority for me to address,” added Rep. Brittany Petterson (D-CO), co-vice chair of the task force. “We have one of the highest suicide rates in Colorado.” She also noted the importance of sustained support for NIH amid the ongoing budget negotiations. “It’s really important for Congress to be here to be reminded of what we’re fighting for.”
Several members come from a science background. Rep. Yadira Caraveo (D-CO), co-vice chair of the task force, is a pediatrician who underscored the need for investments in basic and translational science. Rep. Sean Casten (D-IL), who has a degree in molecular biology and biochemistry, noted his first job was in a colon and breast cancer lab.
NIH Enterprise—an Overview

Photo: Chia-Chi Charlie Chang
The group began the tour in the CC Medical Board Room, where they learned about the inner workings of NIH from leadership. NIH Deputy Director for Management Dr. Alfred Johnson traced NIH’s evolution from a one-room laboratory to the expansive research complex it is today.
Offering a snapshot of NIH’s budget and the funding process, NIH Acting Deputy Principal Director Dr. Tara Schwetz said, “We make funding decisions by considering not just the scientific merit, which of course is critical, but also the scientific opportunity, the public health need and what our portfolio currently looks like.”
Acting NIH Director Dr. Lawrence Tabak highlighted a few of the many contributions NIH has made to improve health. Cardiovascular disease mortality has decreased by 70% in the last six decades, for example. He also noted that cancer death rates are declining more than 1% every year. He pointed out that each 1% drop in cancer mortality saves a staggering $500 billion annually, an example of the immense impact of NIH’s work on both health care and the economy.
In addition, Tabak discussed why NIH investment in rare disease research remains critical.
“If you have the disease, it’s not so rare,” he said. And, “there’s never been a rare disease study that didn’t inform [our understanding of] a widespread disease.”
Tabak also emphasized the importance of diversity in NIH’s research efforts. “Increasingly, I’m asked to defend why diversity matters—it’s about excellence,” he said.
To amplify these efforts, Dr. Marie Bernard, NIH chief officer for scientific workforce diversity, discussed UNITE, an NIH initiative addressing health disparities and fostering diversity and inclusion among the NIH workforce and the extramural research community.
Since 2020, she noted, the nation’s heightened awareness of racial and ethnic disparities has fueled a determination within NIH to drive change. Through dialogue and collaboration, UNITE seeks to ensure all voices are valued toward scientific advancements that benefit all.
In trying to address today’s health challenges, Bernard said, “You’ve got to have people coming at it from a lot of different directions and a lot of experiences.”
After the briefings, the delegation rotated through three NIH labs.
New Tech Key Against Pediatric Cancer

Photo: Chia-Chi Charlie Chang
“Our work focuses on tumors in kids and young adults in which either there’s no standard treatment or the treatments have stopped working,” said Dr. Brigitte Widemann, chief of the National Cancer Institute (NCI) Pediatric Oncology Branch (POB).
In the lab, Dr. Jack Shern, who heads the POB tumor evolution and genomics section, illustrated why developing effective treatments is so complicated in the subset of patients who have a relapse.
A 1-centimeter-cubed piece of tumor might have 100 million cells, he said. Treatment can kill most of those cells but the tiny percentage of malignant cells that returns is refractory.
Shern’s lab does genomic sequencing on tumors to inform and improve treatment. Thanks to new technology, his lab now can get more detailed data using single-cell sequencing.
He described the process: A bar-coded bead goes into a droplet of oil in a microfluidic device. Researchers then feed in cancer cells, one at a time, into that same oil drop. “It ends up in a conical tube that looks like salad dressing,” he said.
“We can now tell differences between sub-populations of cells,” he said. “I’m excited about the possibility of understanding these diseases in a whole new way.”
Support Essential in Recovery
On a second tour stop, Dr. Nora Volkow, director of the National Institute on Drug Abuse (NIDA) and senior investigator in the National Institute on Alcohol Abuse and Alcoholism, described drug addiction as a brain disorder. She shared ongoing research that explores the potential of stimulating or inhibiting specific brain regions to diminish cravings and facilitate the path to recovery.
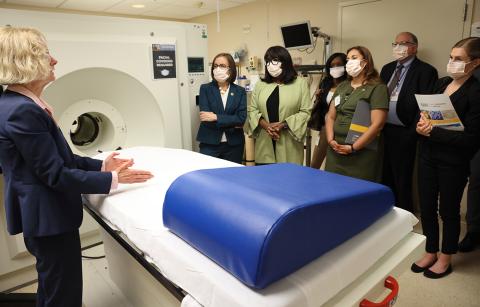
Photo: Chia-Chi Charlie Chang
In studies conducted in Volkow’s lab, MRI and PET scans have revealed significantly reduced activity in the prefrontal areas of the brain among individuals with drug addiction. These regions play a crucial role in executive function and decision-making, shedding light on the neurological basis of addiction’s impact on behavior.
This lab visit proved particularly poignant for Rep. Madeleine Dean (D-PA), who raised concerns about the devastating impact of the fentanyl crisis in her state. She also shared a personal connection.
“I have a son who is 10 years in recovery from opioid addiction,” she said. “I’m hoping in 10 more years that a lot more will be learned. How do we interrupt the overdose death rate now?”
Volkow responded, “The reality is, people who have substance use disorder can recover…it’s not going to happen overnight. You need to provide them with continuous support just as you do for other chronic medical conditions.”
Volkow also highlighted the need for a health care system that addresses addiction at various stages, from early initiation to relapse prevention. Community and social support can further enhance chances of long-term recovery.
Research Gaps Addressed in Youth Mental Health
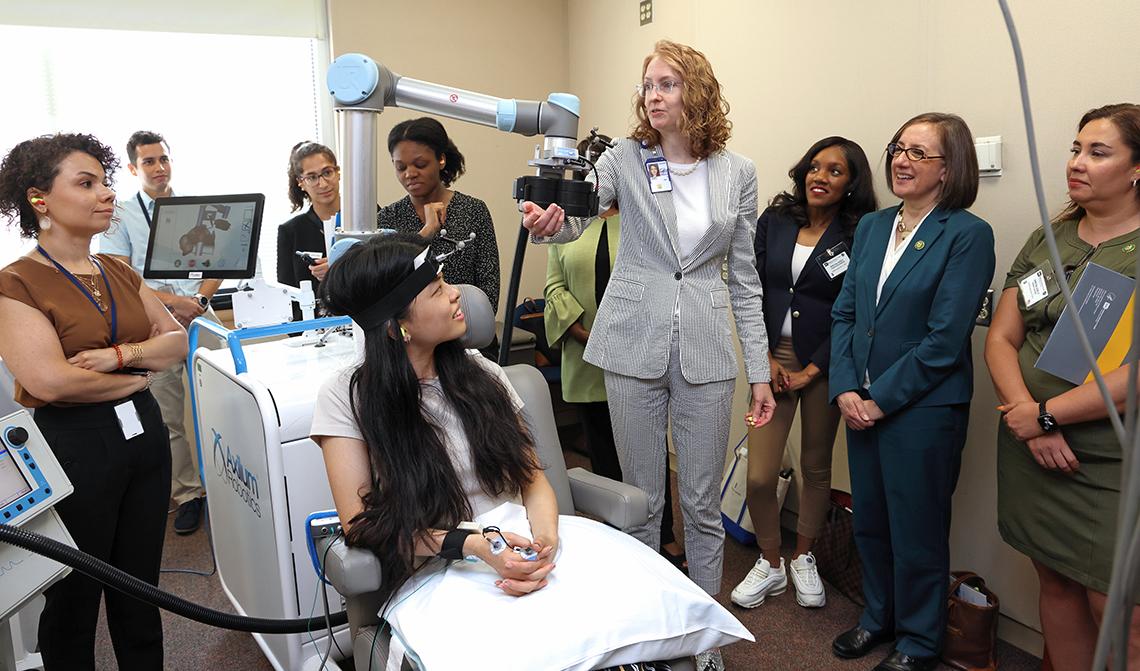
Photo: Chia-Chi Charlie Chang
In a mental health lab, the delegation witnessed a volunteer receiving a noninvasive therapy to stimulate the brain. National Institute of Mental Health Director Dr. Joshua Gordon introduced Dr. Sarah (Holly) Lisanby, head of the noninvasive neuromodulation unit, who demonstrated transcranial magnetic stimulation (TMS) therapy.
The technology enables researchers to study brain function and investigate the roots of psychiatric and addiction disorders toward developing targeted therapies.
Using a robot to navigate the magnetic coil to specific brain regions, the team highlighted the noninvasive nature of TMS, inducing weak electrical currents in the brain to observe and record the effects. The demonstration, which produced a subtle movement in the patient’s hand, illustrated TMS precision and safety.
Lisanby discussed ongoing trials of TMS for autism spectrum disorder and depression in adolescents. Currently, TMS is approved by the Food and Drug Administration to treat depression, obsessive compulsive disorder, smoking cessation and migraine in adults.
“But,” she said, “we know there’s an important unmet need for youth with mental health and substance use disorders, so we’re excited to be addressing those research gap areas.”
As the delegation departed, they had seen firsthand the potential of transformative advances in mental health, substance abuse and cancer, and they left with a deeper understanding of the impact of NIH research.
