NIDDK Celebrates 70 Years of Improving Public Health

Photo: niddk
For 70 years, the National Institute of Diabetes and Digestive and Kidney Diseases has been charged with tackling some of the country’s most serious health problems. And for 70 years, NIDDK staff and grantees have risen to the challenge, bringing talent and dedication to improve prevention, treatment and management of the conditions in the institute’s broad mission.
“The diseases we study cut across the full spectrum of medicine,” said NIDDK director Dr. Griffin Rodgers. “Since its inception in 1950, NIDDK has conducted and supported innovative research that has helped save lives, enhance quality of life and pave the way for future discoveries—discoveries that will continue to improve our nation’s health.”
For example, research advances in diabetes have led to easier and more precise ways for monitoring blood glucose (blood sugar), a critical—but often burdensome—component of disease management.
In 1999, NIDDK-supported research led to the first FDA-approved continuous glucose monitor (CGM), enabling people to track glucose levels in real-time without the need for finger pricks.
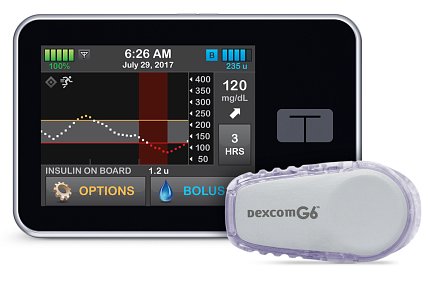
Photo: Tandem Diabetes Care
Today, scientists have taken the CGM a step further with the development of artificial pancreas systems that integrate automated blood glucose management and insulin delivery using an insulin pump. These artificial pancreas devices, the result of incremental discoveries made from years of research supported by NIDDK, could revolutionize both treatment options and health outcomes for people with type 1 diabetes. Hybrid closed loop systems are now commercially available for individuals with diabetes.
NIDDK’s multi-site study, the Diabetes Prevention Program (DPP), has also directly led to type 2 diabetes prevention on a nationwide scale. The study’s results in 2002 showed that moderate weight loss through dietary changes and physical activity, or the drug metformin, can prevent or delay type 2 diabetes in those at high risk for the disease.
Along with grantees, major DPP contributions came from scientists at NIDDK’s Phoenix Epidemiology and Clinical Research Branch in Arizona, who worked with American Indians to ensure they were among the study’s diverse participant pool.
In fact, nearly half of the study participants were from racial and ethnic minority groups, because these groups are at higher risk for type 2 diabetes than the non-Hispanic white population.
“The DPP and its ongoing follow-up in the DPP Outcomes Study have given us an incredible wealth of information by following a diverse group of people early in the course of development of type 2 diabetes,” said Dr. Judith Fradkin, former director of NIDDK’s Division of Diabetes, Endocrinology and Metabolic Diseases, who retired in 2018 after nearly 40 years at NIDDK.

Rodgers concurred. “Many minority and underrepresented groups are disproportionately affected by diabetes and other conditions in NIDDK’s mission,” he said. “As the DPP showed, studies must reflect that diversity for results to be truly applicable and we remain committed to being inclusive in our research efforts.”
Reflecting this commitment, NIDDK’s work in kidney disease has long aimed to better understand the disproportionate burden of kidney disease among black Americans and how to improve health outcomes.
In 2008, research from NIDDK scientists and grantees led to the groundbreaking discovery that variants in a gene called APOL1 are associated with a higher risk of kidney disease and that these variants are found almost exclusively in people of African descent.
Today, the NIDDK-supported APOLLO study, or APOL1 Long-term Kidney Transplantation Outcomes Network, is exploring how these gene variants affect kidney transplantation, with the goal of improving transplant outcomes in both kidney donors and recipients. The study enlisted an advisory committee of black Americans with kidney disease to ensure that the people most affected by the findings have a key role in the research process.
The APOLLO study exemplifies a core tenet of NIDDK’s philosophy: putting the people it serves at the center of its research.

Photo: Laurie Russell, Wake Forest University
“The key is to realize that it’s not about you, it’s about everybody else that you’re serving,” said Dr. Allen Spiegel, NIDDK director (1999-2006), in a 2019 oral history. “If you keep that in mind, you can be successful.”
Some of NIDDK’s most notable successes have been in liver research, including the Nobel Prize-winning discovery of the hepatitis B virus by an NIDDK scientist, and the first successful human liver transplantation, performed by an NIDDK grantee.
Research advances led to a vaccine for hepatitis B, available since 1982, which has greatly reduced the disease’s prevalence.
Scientists at NIDDK also tested the first effective therapy for chronic hepatitis C in the 1980s, and more recently, NIDDK-funded research has helped identify several direct-acting viral drugs being used to treat—and cure—hepatitis C. NIDDK scientists are now working to develop a hepatitis C vaccine, which, if successful, could help dramatically reduce the virus’ spread.
These and countless other achievements across the institute reflect the dedication of scientists—both intramural and extramural—and of NIDDK staff, who all share the vision of improving public health.
“At NIDDK, one of the enormous resources is the quality of people, not only the scientists, but all the people who work on grants, who help maintain this whole community that we’ve developed through thick and thin,” said Dr. Phillip Gorden, NIDDK director (1986-1999) and current senior investigator, in his oral history.
This spirit of collaboration and service across NIDDK has helped shape the institute over the past 70 years and will continue to fuel its progress in the years to come.
