Various Aspects of Attack
Covid-19 Affects Heart, Other Organs

Covid-19 is not just a respiratory virus. The virus affects many organs, including the heart, said Dr. Eric Topol during a recent NHLBI webinar series called “Covid-19 Insights.”
“The more we learn about Covid, the more we learn about other aspects of its attack,” said Topol, executive vice president and professor of molecular medicine at Scripps Research Institute and founder and director of the Scripps Research Translational Institute.
Coronaviruses are spherical viruses that have crown-like protein spikes on their surfaces. The spikes found on SARS-CoV-2, the virus that causes Covid-19, bind to a protein called ACE2, which is located on the surface of cells found in the lungs, heart, arteries and other organs. This binding allows the virus to enter and take over the cell.
New strains of the virus are emerging, Topol warned. One strain, called B.1.1.7, is a “hyper transmissible super-spreader variant” and it’s present in the United Kingdom and Ireland. How these new strains differ from established strains isn’t well known yet.
“It’s the worst thing to have a strain with 50 percent more transmission,” he said. “Even without any increase in lethality from the strain per se, the high incidence of infections will lead to much more in the way of hospitalizations and deaths.”
The virus affects people in different ways. A few people are never infected despite being exposed; 30-40 percent of those infected with the virus are asymptomatic—that is, they never experience symptoms. Fortunately, most people who develop symptoms don’t become seriously ill. A small fraction of patients become critically ill and require hospitalization. In some cases, the illness is fatal.
A tiny fraction of patients experience serious cardiovascular complications, including the scarring and thinning of the heart muscle, myocarditis, cardiomyopathy, arrythmias and cardiac arrest. But Covid-19 can cause damage even in asymptomatic patients. It’s not yet known how heart damage occurs—whether from the virus directly attacking heart cells or from the immune system’s response to the virus. Figuring out how the heart damage happens will help researchers develop better treatments.
“There’s a whole spectrum of things the virus does to the heart and the blood vessels,” Topol said. “We don’t know why certain people are predisposed.”
Another rare, but serious condition associated with Covid-19 is multisystem inflammatory syndrome in children (MIS-C). In MIS-C, different body parts, such as the heart, lung, kidneys, brain, skin and eyes, become inflamed. It’s fatal in 1-2 percent of children.
While the fatalities are “horrific,” he argued, not enough attention has been paid to patients experiencing long-term symptoms of Covid-19. These include chronic fatigue, chest pain, shortness of breath, dyspnea and a decreased ability to perform physical exercise. This is occurring in at least 10-20 percent of people. Those who experience long-term symptoms tend to be young, female and previously healthy.
“Studies suggest it goes on in most people for many months,” he said. “We don’t even know the real duration because this is only a 1-year old disease. It may go on for years.”
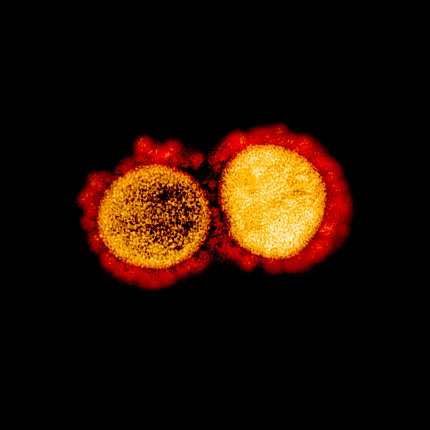
Photo: NIAID
In the future, artificial intelligence technologies might be used to accurately diagnose Covid-19. Recently, researchers built an algorithm to identify cases based on the sound of a person’s cough. In a study of more than 4,000 people, the algorithm provided an accurate diagnosis 98.5 percent of the time.
Topol cautioned that while there is potential, few AI studies have been fully replicated. A lot more work must be done before these technologies can be used widely.
Sensor data from wearable technologies could help find new infections.
In a study of 40,000 participants, Topol led a team that collected and analyzed data from smartwatches and activity trackers. They found people who are beginning to develop symptoms have a higher resting heart rate, a decrease in steps and an increase in sleep.
“We think we can use this to detect Covid-19 outbreaks early,” he concluded. “We’re hoping to scale this up. We think this could be useful because we can then go in aggressively and do testing and isolation and get a much better containment of the virus.”
