Brooks Narrows Search for Therapeutics for Albinism-Related Vision Loss

Vision impairment is a common feature in most individuals with albinism, a condition in which the skin, hair and eyes (or some combination of the three) have reduced melanin pigmentation. Problems with eyesight can be so severe that people may be declared legally blind. Dr. Brian P. Brooks of NEI is investigating therapies to improve vision quality in patients with oculocutaneous albinism (OCA), which is the most common form of albinism in the U.S.
Generally, “the less melanin is present, the worse vision tends to be,” Brooks said in a recent Clinical Center Grand Rounds Lecture. Affected individuals have lower than normal visual acuity and are also more sensitive to light and glare because of their lack of pigmentation.
Albinism is an inherited condition, and there are multiple forms found throughout the world. Brooks focuses his research on OCA1, the most common form in North America. Individuals with this form of albinism have mutations in their tyrosinase gene. There are two subtypes of OCA1: OCA1A, in which patients have no tyrosinase activity, and OCA1B, in which patients have some tyrosinase activity.
Melanin is synthesized from the amino acid tyrosine, so a lack of tyrosine corresponds to a lack of melanin pigment. Tyrosinase, the enzyme that metabolizes tyrosine in the first step of melanin production, is either not produced at all or only made in small quantities.
Because tyrosinase is at the beginning of the melanin synthetic pathway, Brooks explained, a decrease in activity would be expected to affect both eumelanin (black/brown pigment) and pheomelanin (red/yellow pigment) in melanocytes, the cells that produce melanin.
Brooks’s study found a trend where eumelanin was increased more than pheomelanin in the hair of participants after drug treatment. A higher eumelanin/pheomelanin ratio may help protect people with albinism from developing skin cancer.
Most treatment for vision loss caused by albinism is only supportive. If there was a treatment to improve melanin pigmentation in patients with albinism, Brooks wondered, would that improve their vision function?
Melanin is found in the iris, retinal pigment epithelium (RPE) and choroid of the eye, and the lack of these pigments contributes to vision problems. Ideally, treatment would focus on identifying and treating affected individuals while still in utero, as the eyes develop, or in the first few years after birth as the eyes finish maturing.
Brooks identified the drug nitisinone (NTBC) as a potential treatment. It blocks tyrosine degradation, and he hypothesized that it would elevate tyrosine levels in patients with albinism, which would stabilize tyrosinase and allow it to increase melanin synthesis.

He first studied NTBC in mice, with promising results. Partly albino Himalayan mice represented OCA1B patients, and fully albino mice represented OCA1A patients. Young mice were fed NTBC for several months, and the OCA1B group developed darker skin pigmentation. The fully albino group showed no increase in skin pigment. The partly albino group also had a slight increase in iris pigmentation when viewed under a microscope.
A closer look at the RPE, iris and choroid showed no change in the mature melanosomes (produced by melanocytes) that are responsible for producing melanin in the OCA1A mice, but a demonstrable increase in the OCA1B mice. Daily NTBC supplementation for pregnant OCA1B mice produced young that had darker fur and eyes than their parents.
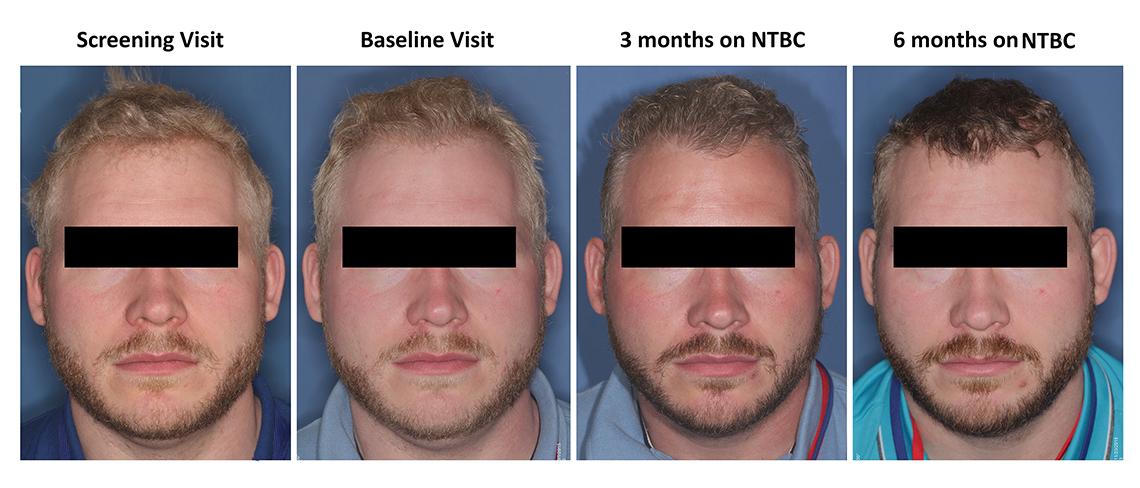
After studying NTBC in mice, Brooks completed a 1-year pilot study of the drug in 5 patients with OCA1B (3 women and 2 men). He did not expect the drug to increase visual acuity in adults because of their mature visual system but expected to see some increase in melanin pigmentation. Study subjects were given a daily dose of NTBC; their hair, skin and eye pigmentation were monitored.
Responses varied on an individual basis, but there was a general increase in skin and hair melanin during the 1-year course of NTBC. Researchers did not observe a clinically significant increase in visual acuity, but believe that NTBC might produce better results in children because their visual systems are not fully developed.
In terms of future research, Brooks and his team are working to identify new compounds that may be useful for increasing tyrosine in the body, and are also looking into therapies that target the RPE.
In collaboration with Dr. Kapil Bharti of NEI’s ocular and stem cell translational research section, Brooks and his team have isolated blood cells from 2 patients with OCA1A and 2 with OCA1B and converted those cells to pluripotent stem cells. These new cells are then given cues to differentiate into RPE cells, which can be studied in the lab. They exhibit all the characteristics of cells with albinism, and will be important for identifying new therapies.
View the entire lecture at https://videocast.nih.gov/watch=42286.
