Vision Improves with Treatment for Blinding Blood Vessel Condition
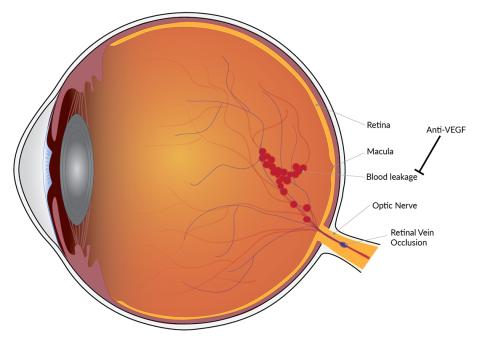
Photo: NEI
New research shows that a treatment for retinal vein occlusion (RVO) yields long-lasting vision gains, with visual acuity remaining significantly above baseline at 5 years. However, many patients require ongoing treatment.
RVO is one of the most common blinding conditions in the U.S. Without treatment, central retinal vein occlusion (CRVO), the most severe type, often leads to significant and permanent vision loss.
A report on 5-year outcomes of the Study of Comparative Treatments for Retinal Vein Occlusion 2 (SCORE2), was published in the American Journal of Ophthalmology. SCORE2 was funded in part by NEI.
RVO is caused by a blockage of the veins carrying blood away from the retina, which can lead to rapid and severe loss of visual acuity. The most effective treatment, injections of anti-vascular endothelial growth factor (VEGF) drugs, helps control blood vessel leakage and swelling in the retina.
In 2017, SCORE2 clinical trial investigators reported that two types of anti-VEGF treatment were equally effective at improving visual acuity in people with macular edema due to RVO.
Half of the study participants received Avastin (bevacizumab) while the other half received Eylea (aflibercept). Both drugs were injected monthly. At the 6-month mark, the vision of participants in both groups had, on average, improved over 3 lines on an eye chart.
After the initial 12-month study period, most physicians reduced the frequency of anti-VEGF injections and some switched their patients to the other anti-VEGF drug. At 5 years, many participants had lost some visual acuity compared to their 12-month checkup; however, they retained on average 3 lines of improvement.
Study chair Dr. Ingrid Scott of Penn State College of Medicine said the study “underscores the importance of disease monitoring and individualized treatment to achieve the best possible vision.”
